Alkaptonuria: pathogenesis, clinical manifestations, and management perspectives
 DOI:
DOI:
https://doi.org/10.33974/jjj9az89
Keywords:
Alkaptonuria , Homogentisic acid, Ochronosis, Nitisinone, ArthropathyAbstract
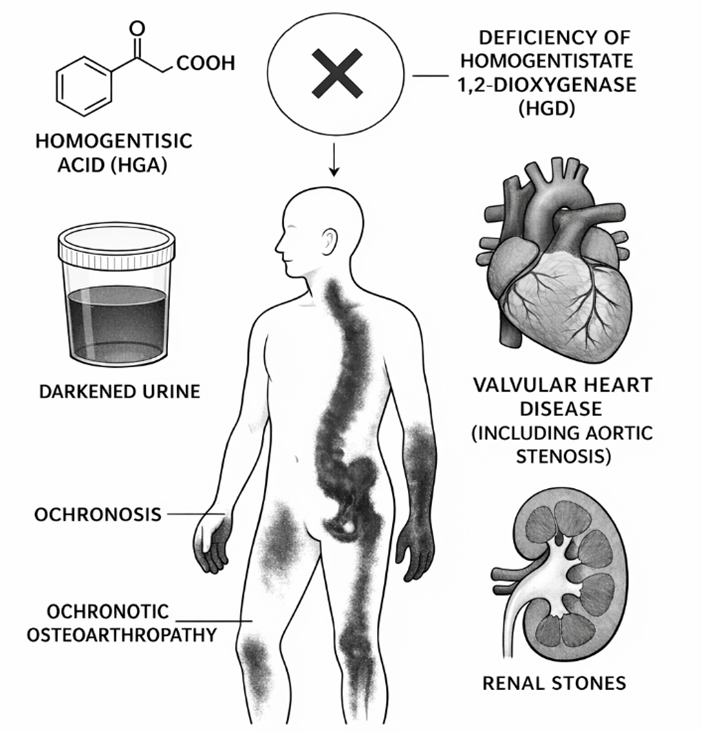
Alkaptonuria (AKU) is a rare autosomal recessive disorder caused by mutations in the HGD gene, leading to deficiency of homogentisate 1,2-dioxygenase and accumulation of homogentisic acid (HGA). Oxidized HGA forms ochronotic pigment that deposits in connective tissues, producing progressive damage. The earliest sign is urine darkening. Over time, bluish-brown discoloration of cartilage, spinal stiffness, large-joint arthritis, tendon ruptures, aortic valve disease, and renal calculi may develop. The global prevalence ranges from 1 in 25,000 to 1 in 1,000,000 births, with higher incidence in Slovakia, the Dominican Republic, India, and Jordan. Diagnosis is confirmed by urinary HGA measurement via high-performance liquid chromatography, HGD mutation analysis, and imaging such as MRI, CT, or DEXA.Treatment is mainly supportive, including analgesics, physiotherapy, and surgery for severe joint involvement. Nitisinone therapy significantly reduces urinary HGA and may slow disease progression but requires monitoring of plasma tyrosine levels. Although AKU rarely reduces lifespan, it causes substantial morbidity, highlighting the importance of early detection, multidisciplinary management, and further research into disease-modifying therapies.
Downloads
References
Zatkova, A., Ranganath, L., & Kadasi, L. (2020). Al-kaptonuria: Current Perspectives. The Application of Clinical Genetics, 13, 37–47. https://doi.org/10.2147/TACG.S186773
Bernardini, G., Braconi, D., Zatkova, A., Sireau, N., Kujawa, M. J., Introne, W. J., Spiga, O., Geminiani, M., Gallagher, J. A., Ranganath, L. R., & Santucci, A. (2024). Alkaptonuria. Nature Reviews Disease Primers, 10(1), 1–15. https://doi.org/10.1038/s41572-024-00498-x
Mistry, J. B., Bukhari, M., & Taylor, A. M. (2013). Alkaptonuria. Rare Diseases, 1(1). https://doi.org/10.4161/rdis.27475
Davison, A. S., Milan, A. M., Gallagher, J. A., & Ranganath, L. R. (2015). Acute fatal metabolic complications in alkaptonuria. Journal of Inherited Metabolic Disease, 39(2), 203–210. https://doi.org/10.1007/s10545-015-9902-0
Davison, A., Hughes, A., Milan, A., Sireau, N., Gal-lagher, J., & Ranganath, L. (2019). Alkaptonuria – Many questions answered, further challenges beckon. Annals of Clinical Biochemistry: Interna-tional Journal of Laboratory Medicine, 57(2), 106–120. https://doi.org/10.1177/0004563219879957
Ranganath, L. R., Taylor, A., A. Shenkin, Fraser, W. D., Jarvis, J. C., Gallagher, J. A., & N. Sireau. (2011). Identification of alkaptonuria in the general popu-lation: a United Kingdom experience describing the challenges, possible solutions and persistent bar-riers. Journal of Inherited Metabolic Disease, 34(3), 723–730. https://doi.org/10.1007/s10545-011-9282-z
Srsen, S., Müller, C. R., Fregin, A., & Srsnova, K. (2002). Alkaptonuria in Slovakia: thirty-two years of research on phenotype and genotype. Molecular Genetics and Metabolism, 75(4), 353–359. https://doi.org/10.1016/s1096-7192(02)00002-1
Yang, Y., Guo, J., Chen, W., Zhao, R., Tang, J., Meng, X., Zhao, L., Tu, M., He, X., Wu, L., & Zhu, Y. (2013). First report of HGD mutations in a Chinese with al-kaptonuria. Gene, 518(2), 467–469. https://doi.org/10.1016/j.gene.2013.01.020
Ayse Ergul Bozaci, Havva Yazici, Canda, E., Sema Kalkan Uçar, Merve Saka Guvenc, Afig Berdeli, Habif, S., & Coker, M. (2022). Long-term follow-up of alkaptonuria patients: single center experience. Journal of Pediatric Endocrinology and Metabo-lism, 35(7), 913–923. https://doi.org/10.1515/jpem-2022-0004
Davison, A. S., Milan, A. M., Gallagher, J. A., & Ranganath, L. R. (2015). Acute fatal metabolic complications in alkaptonuria. Journal of Inherited Metabolic Disease, 39(2), 203–210. https://doi.org/10.1007/s10545-015-9902-0
Wu, K., Bauer, E., Myung, G., & Fang, M. A. (2018). Musculoskeletal manifestations of alkaptonuria: A case report and literature review. European Journal of Rheumatology. https://doi.org/10.5152/eurjrheum.2018.18116
Norman, B. P., Sutherland, H., Wilson, Rutland, D. A., Milan, A. M., Hughes, A. T., Davison, A. S., M. Khedr, Jarvis, J. C., Gallagher, J. A., G. Bou‐Gharios, & Ranganath, L. R. (2024). Hepatobiliary circula-tion and dominant urinary excretion of homo-gentisic acid in a mouse model of alkaptonuria. Journal of Inherited Metabolic Disease. https://doi.org/10.1002/jimd.12728
Grosicka, A., & Kucharz, E. J. (2009). Alkaptonuria. Wiadomosci Lekarskie (Warsaw, Poland: 1960), 62(3), 197–203. https://pubmed.ncbi.nlm.nih.gov/20229718
Braconi, D., Millucci, L., Bernardini, G., & Santucci, A. (2015). Oxidative stress and mechanisms of ochronosis in alkaptonuria. Free Radical Biology and Medicine, 88, 70–80. https://doi.org/10.1016/j.freeradbiomed.2015.02.021
Borman, P., Bodur, H., & Cılız, D. (2002). Ochrono-tic arthropathy. Rheumatology International, 21(5), 205–209. https://doi.org/10.1007/s00296-002-0175-1
J.F. Van Offel, Luc, Francx, L. M., & Stevens, W. J. (1995). The Clinical Manifestations Of Ochronosis: A Review. Acta Clinica Belgica, 50(6), 358–362. https://doi.org/10.1080/17843286.1995.11718475
Chu, P., Cuellar, M. C., Bracken, S. J., & Tarrant, T. K. (2021). A Mimic of Ankylosing Spondylitis, Ochronosis: Case Report and Review of the Litera-ture. Current Allergy and Asthma Reports, 21(3). https://doi.org/10.1007/s11882-021-01002-1
Ranganath, L. R., Khedr, M., Vinjamuri, S., & Gal-lagher, J. A. (2020). Frequency, diagnosis, patho-genesis and management of osteoporosis in alkap-tonuria: data analysis from the UK National Alkap-tonuria Centre. Osteoporosis International. https://doi.org/10.1007/s00198-020-05671-y
Braconi, D., Bernardini, G., Alessandro Paffetti, Millucci, L., Michela Geminiani, Laschi, M., Fredi-ani, B., Marzocchi, B., & Santucci, A. (2016). Com-parative proteomics in alkaptonuria provides in-sights into inflammation and oxidative stress. The International Journal of Biochemistry & Cell Biolo-gy, 81, 271–280. https://doi.org/10.1016/j.biocel.2016.08.016
Fishberg, E. H. (1942). The instantaneous diagno-sis of alkaptonuria on a single drop of urine. Jama: The Journal of the American Medical Association, 119(11), 882. https://doi.org/10.1001/jama.1942.72830280001009
Vinjamuri S., Ramesh C., Jarvis J.C., Gallagher J.A., Ranganath L.R. (2011). Nuclear medicine tech-niques in the assessment of alkaptonuria. Nuclear Medicine Communications, 32(10), 880–886. https://doi.org/10.1097/mnm.0b013e32834955df
Bassily, E., O’Dell, M. C., Homan, B., & Wasyliw, C. (2016). Alkaptonuria. Orthopedics, 39(4). https://doi.org/10.3928/01477447-20160503-03
Gil, J. A., Wawrzynski, J., & Waryasz, G. R. (2016). Orthopedic Manifestations of Ochronosis: Patho-physiology, Presentation, Diagnosis, and Manage-ment. The American Journal of Medicine, 129(5), 536.e1–536.e6. https://doi.org/10.1016/j.amjmed.2016.01.010
Tinti, L., Adriano Spreafico, Braconi, D., Millucci, L., Bernardini, G., Chellini, F., Cavallo, G., Enrico Selvi, Galeazzi, M., Marcolongo, R., Gallagher, J. A., & Santucci, A. (2010). Evaluation of antioxidant drugs for the treatment of ochronotic alkaptonuria in an in vitro human cell model. Journal of Cellular Physiology, 225(1), 84–91. https://doi.org/10.1002/jcp.22199
Ranganath, L. R., Psarelli, E. E., Arnoux, J.-B., Braconi, D., Briggs, M., Bröijersén, A., Loftus, N., Bygott, H., Cox, T. F., Davison, A. S., Dillon, J. P., Fisher, M., FitzGerald, R., Genovese, F., Glasova, H., Hall, A. K., Hughes, A. T., Hughes, J. H., Imrich, R., & Jarvis, J. C. (2020). Efficacy and safety of once-daily nitisinone for patients with alkaptonuria (SONIA 2): an international, multicentre, open-label, randomised controlled trial. The Lancet. Di-abetes & Endocrinology, 8(9), 762–772. https://doi.org/10.1016/S2213-8587(20)30228-X
Milella, M. S. (2022). Study of molecular mecha-nisms and pharmacological approaches of Alkap-tonuria’s disease. Doi.org. https://doi.org/10.25434/milella-maria-serena_phd2022
Ranganath, L. R., Jarvis, J. C., & Gallagher, J. A. (2013). Recent advances in management of alkap-tonuria (invited review; best practice article). Journal of Clinical Pathology, 66(5), 367–373. https://doi.org/10.1136/jclinpath-2012-200877
Drakoulakis, E., Varvitsiotis, D., Psarea, G., & Feroussis, J. (2012). Ochronotic arthropathy: diag-nosis and management: a critical review. American Journal of Orthopedics (Belle Mead, N.J.), 41(2), 80–83. https://pubmed.ncbi.nlm.nih.gov/22482092
Ramesh K., Jayaram N., Vinoth R., Getzy Immacu-late P.A., Jagan M., Nepolean R. (2025). Immuno-logical Insights and Therapeutic Innovations in Atopic Dermatitis: A Contemporary Review. Jour-nal of Advances in Pharmacy Practices, 7(2), 1–9.
K Ramesh, R Vinoth, N Jayaram, S Sivasankari, S Nagajothy, R Sapthasri. (2025). The Synergy of Immunology and Precision Medicine in Therapeu-tic Revolution of Rheumatoid Arthritis. PriMera Scientific Surgical Research and Practice, 6(3), 05–12.
Ramesh K., Gnana Sree G., Priyadharshini K., Shalini Antonia S., Nepolean R. (2025). Cystinosis: Unravelling Molecular Mechanisms, Clinical Chal-lenges, and Therapeutic Innovations. Journal of Pharmaceutical Sciences, 1(11), 153–159. https://doi.org/10.5281/zenodo.17510169.
Ramesh K., Jerome Thomson, Mohamed Jalalu-deen, Gurucharan P., Pradheep K., Nepolean R. (2025). Advances in Asthma Management: Integrat-ing Biologics, Nanotechnology, Digital Health, and Precision Medicine. World Journal of Pharmaceuti-cal Research, 14(21), 1204–1229.
Ramesh Kumar, Haritha Rajangam, Hemalatha Muthaiyah, Chinjumol Millus, Venmathi Viswana-than, Nepolean Ramasamy. (2026). A Comprehen-sive Clinical and Therapeutic Review of Achondro-plasia and Related Skeletal Dysplasias. Med Pharm Journal, 4(4), 263–267. https://doi.org/10.55940/medphar2025170.
Downloads
Published
Issue
Section
License
Copyright (c) 2026 Ramesh K, Nepolean R, Vinothkumar S, Baskar N, Hemalatha M, Chinjumol ML, Haritha RR, Shobana A (Author)

This work is licensed under a Creative Commons Attribution-ShareAlike 4.0 International License.
License Terms
This is an open-access article published in the International Journal of Research in Pharmaceutical Sciences and Technology (IJRPST) by Rubatosis Publications.
It is distributed under the terms of the Creative Commons Attribution 4.0 International License (CC BY 4.0), which permits unrestricted use, distribution, reproduction, and adaptation in any medium or format, provided the original author(s) and source are appropriately credited, a link to the license is provided, and any changes made are indicated.
To view a copy of this license, visit: https://creativecommons.org/licenses/by/4.0/
For any further queries or permissions beyond the scope of this license, please contact: editor@rubatosis.org





